ICSI
IVF Treatment
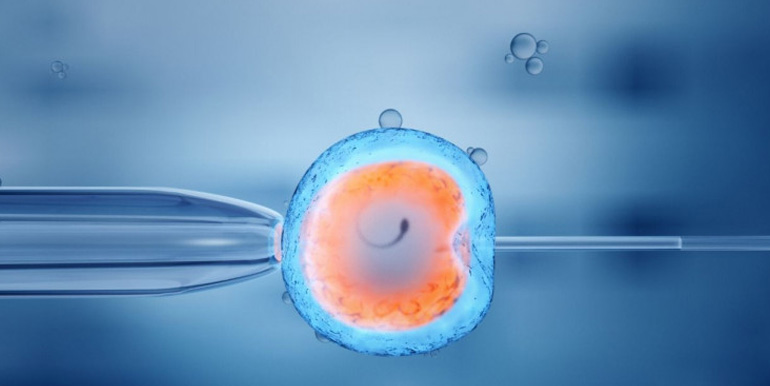
Intracytoplasmic sperm injection (ICSI) is a technique used in IVF that fertilizes an egg with a pre-selected sperm. ICSI is performed by an embryologist in the laboratory, under the guidance of a microscope. This helps to enable fertilization in cases where sperm have a low chance of fertilizing an egg on their own. Even when there are only a few sperm available, an embryologist can select the best sperm and directly insert it into the egg to fertilize it. High success rates with this procedure have revolutionized the treatment of male infertility. ICSI has very high and constant success rates to achieve fertilization (70-80%)Sperm motility and the experience of the embryologist applying the technique are two of the most important parameters to guarantee its effectiveness.
In a normal IVF cycle without ICSI, eggs and sperm are mixed in a petri dish and fertilization occurs spontaneously in the dish. In contrast, in an IVF cycle utilizing ICSI, an embryologist selects the best sperm from a semen sample using a microscope and injects the sperm directly into an egg.
WHEN IS ICSI RECOMMENDED?
1. Male infertility:
- Oligozoospermia or cryptozoospermia: A severely low sperm count
- Astenozoospermia: Severely low sperm motility, including samples with a total lack of motility.
- Teratozoospermia: A high number of abnormal sperm.
- Obstructive azoospermia: A total absence of sperm in the ejaculate due to an obstruction. The most common causes are genetic disorders, inflammation and failed vasostomy.
- Testicular azoospermia: A total absence of sperm in the ejaculate due to a disorder of sperm production in the testicles.
- Anejaculation: Ejaculatory dysfunction caused by retrograde ejaculation or paraplegia.
- In cases of azoospermia and anejaculation, the sperm needed for ICSI can be retrieved directly from the testicles (by testicular puncture or biopsy) (tese)
- Immune cause: Presence of high levels of anti-sperm antibodies.
- Valuable sperm samples: Patients, who freeze their sperm sample before undergoing chemotherapy or radiotherapy, patients that require sperm washing due to an infectious disease (HIV, hepatitis) or use of donor semen.
2. Female infertility:
- Low oocyte count is retrieved after the follicles are punctured. Under such circumstances, standard IVF can be performed.
- The quality of oocytes is low in general including the swollen oocyte coat (zona pellucida).
3. Other causes:
- Long term infertility (more than 2 years of trying to conceive)
- Several unsuccessful cycles of times intercourse or artificial insemination.
- Not performing standard IVF in the previous cycle.
- Rescue microinjection: oocyte microinjection for the failure in the fertilization after standard IVF.
- In Vitro Oocyte Maturation.
- Failing to conceive after several standard IVF cycles.
- Vitrified oocyte microinjection.